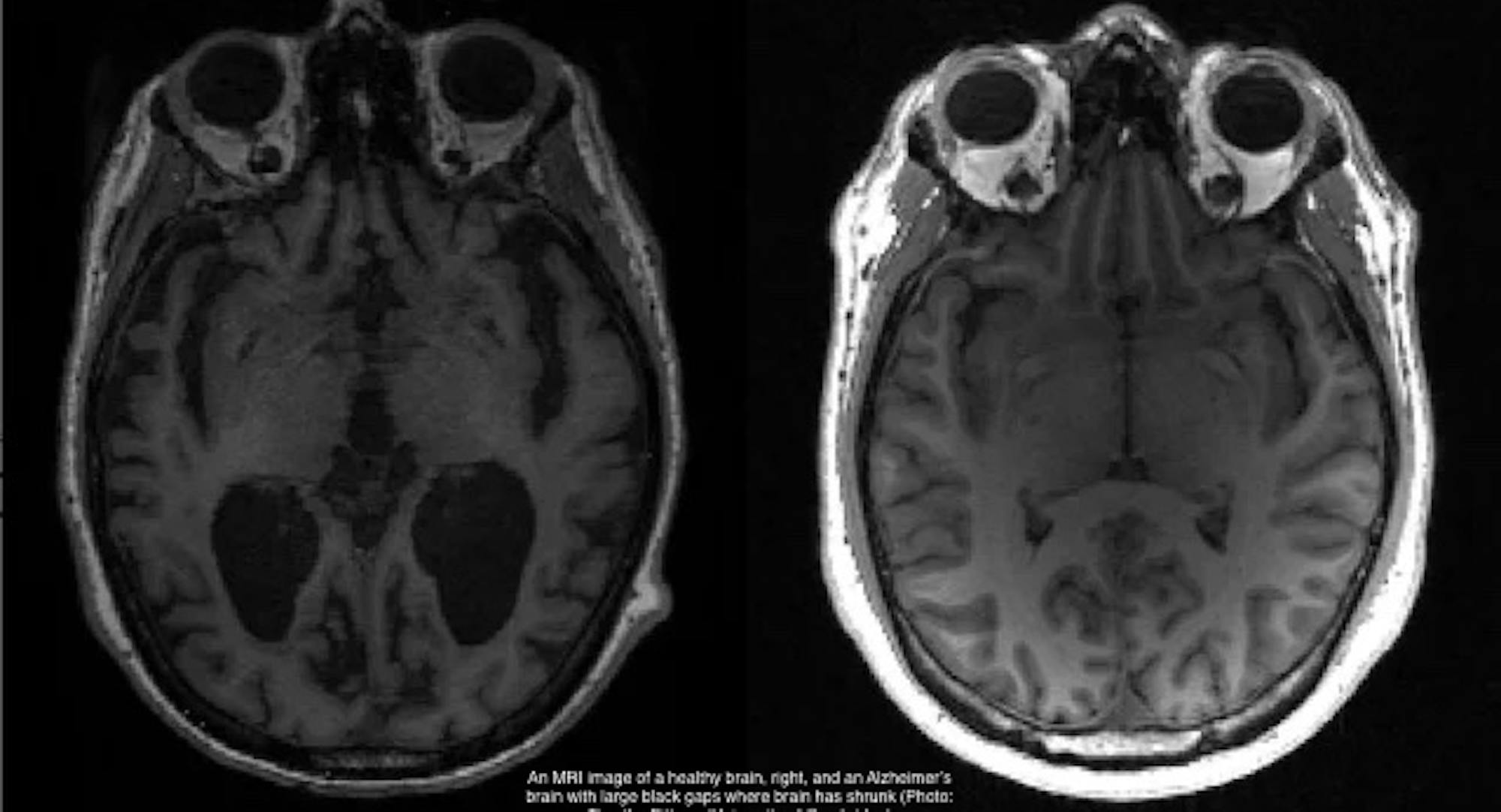
This section contains extracts from the book How Not to Study a Disease – The Story of Alzheimer’s (Chapter 1) by Karl Herrup. It has been edited for the purposes of this article.
DOROTHY’S STORY
Dorothy's story serves as a poignant reflection of the devastating reality of Alzheimer's Disease. Recounted by her daughter, it reveals how this cruel condition gradually stole away Dorothy’s vibrant personality, causing heartache and stress for the entire family.
Dorothy led an active life, but her decline became evident in her late 80s when she started getting lost while driving. Eventually, she had to move to an assisted living facility as her condition worsened. She experienced memory lapses that made her forget significant events, like wearing a new pair of shoes. Her daughter recognised these signs as serious problems. While doctors diagnosed her with Alzheimer's or some form of dementia, the medication had limited effect.
Dorothy's decline persisted for almost eight years until she died peacefully at the age of 96. Her story exemplifies both typical and atypical aspects of Alzheimer's disease, highlighting the variable and complex nature of this devastating condition.
“Listening to Dorothy's daughter recounting her mother's journey evoked powerful emotions within me, as it does for many researchers working towards finding a cure for this disease. It also brought to light the fear that individuals face when confronted with the possibility of Alzheimer's affecting their own lives and their families. Dorothy's daughter perceived Alzheimer's as a disease of the brain, but, to her, it primarily represented a source of heartache and stress. Watching her mother's presence fluctuate unpredictably took a toll on her own energy, patience, and strength”.
Dorothy was popular among her friends, rarely missed a crossword puzzle, walked everywhere to stay physically active, travelled extensively, and maintained strong connections with her social group after the untimely loss of her husband. Engaging in politics and civic duties, she possessed contagious laughter and an appreciation for humour that drew people towards her.
“The first hint that something was amiss occurred in Dorothy's late 80s when a friend expressed concern over her increasing tendency to get lost while driving. Subsequently, minor accidents heightened worry, prompting her daughter to take action. Convincing Dorothy to stop driving and transition to an assisted living facility marked the realisation that something was wrong”.
Dorothy's condition worsened during her stay at an assisted living facility. Medical professionals confirmed the presence of Alzheimer's or related dementia through diagnostic tests. Attempts with medications showed limited effectiveness and unwanted side effects. As Dorothy's dependency increased, she was moved to a more intensive assisted living setup, where she encountered unnecessary obstacles and a lack of personalised care.
“Language was next. Dorothy’s ability to remember and use words slowly but surely started going, especially, the daughter said, after she moved to the new unit. She came in as one of the more “high-performing” folks but quickly went downhill. And, perhaps as a result, the staff started doing less and less for her, which in turn only seemed to make things worse. Her motor abilities declined, and she had to use a wheelchair. “She never forgot how to eat, though,” her daughter told me. “And the best thing was, she never forgot who I was. Most of her words were gone, but when I came in, she would always grin and raise her arms up and say, ‘Yay.’” At this point, she liked simple pleasures, the daughter told me. They would go through art books together and look at the pictures or listen to Frank Sinatra together and sometimes sing along. The staff seemed to like Dorothy despite her limitations. She would occasionally have a nasty exchange with one of the caregivers, but she was never truly aggressive with them or with other persons in the facility. One day, after nearly two years in this memory unit, the daughter went to see her mother before leaving for a trip. “She was different…,”
Dorothy spent over a decade navigating the increasing symptoms of her disease. Her daughter was 70 years old when the author interviewed her—those years represented a significant amount of time when stress, trauma and complications became an everyday occurrence. Dorothy's daughter's account highlights not only the personal toll of Alzheimer's Disease but also the profound impact it has on families. The heartache, stress, and energy required to navigate the relentless changes and shifting needs of their loved ones are immense.
When we consider that Dorothy’s experience was by no means isolated, there remain some sobering questions.
Could the pursuit of a ‘cure’ for Alzheimer's Disease instil false hope for patients and their families?
Can we expect current and future therapies to work consistently with all patients?
If a specific therapy can fully stop progression, is that considered a cure? Or do we need to revert back to an appropriate level of cognitive function to conclude we have a cure finally?
As we honour Dorothy's memory, let us remember that her story represents a collective struggle faced by those affected by Alzheimer's Disease. It serves as a call to action, motivating researchers, healthcare professionals, and society as a whole to intensify their efforts in finding effective treatments and support systems to come as close to finding a cure as possible. By embracing the complexity and variability of this disease, we can foster compassion, understanding, and progress in the fight against Alzheimer's.
Finding a ‘Cure’ for Alzheimer’s Disease
In Jason Karlawish's inspiring book, "The Problem of Alzheimer's," Chapter 22 delves into the significance of hope within a comprehensive plan. He astutely points out that Alzheimer's Disease represents the least common variant of the disorder (p.229). Given the intricate nature of this disease, can we realistically anticipate finding a definitive cure? Is it within reach?
In the same enlightening chapter, Karlawish references George Vrandenburg's 2017 interview, where Vrandenburg emphasised the need for high-quality care institutions for an extended period, even if we develop some effective drugs (p.230). Vrandenburg likens addressing the Alzheimer's crisis solely through pursuing a cure to relying solely on lottery tickets to plan for retirement (p.230).
Within the pharmaceutical and medical field, witnessing the rapid advancements in potential Alzheimer's Disease treatments is undeniably thrilling and fills us with hope. In the real world, though, glamorous headlines, overly optimistic claims and questionable decisions surrounding the approval of products may well be doing more harm than good. We must acknowledge that expecting a solitary, simplistic "cure" may generate false hope among those hit hardest. The road ahead for Alzheimer's Disease is lengthy, and we must comprehend that it is not a one-size-fits-all affliction. Exploration of a multitude of treatment options is likely. A pragmatic approach to assessing the tangible benefits these therapies yield for actual patients beyond the confines of the laboratory setting is vital.
With all of this in mind, how do we go beyond the numerical value of efficacy endpoints? Or better yet, why do we need to? The latter is obvious - We need to keep the patients’ experiences and realities in mind when discussing Alzheimer’s Disease treatments - but the former? That is for you to decide.